She also strongly insisted on returning to the marital home and did so. These potential risks were explained to her and the husband, but consent to immediate admission could not be obtained. 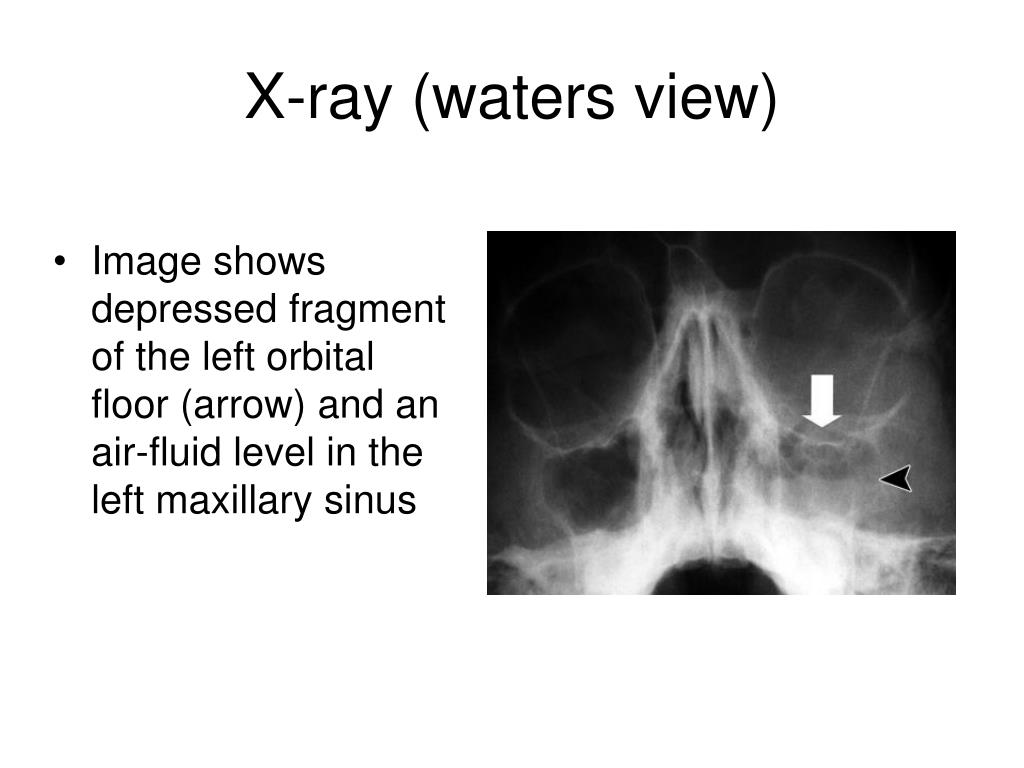
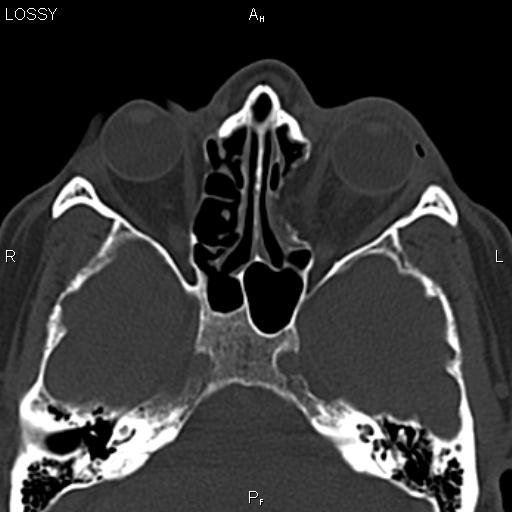
These findings raised concerns that orbital cellulitis could progress to intracranial infection unless intensive treatment was started. It was noteworthy that there was no new blowout fracture. Orbital CT also showed that the shape of eyeball was maintained and that there was neither foreign body nor abscess in the orbit. Head CT showed the old blowout fracture and chronic sinusitis as observed previously, but also orbital cellulitis and maxilla fracture that had not been previously detected. There was no obvious bruising around the eye and no tear on the ocular surface at that time. Although antianxiety and antipsychotic drugs were used under the direction of a psychiatrist as she started having a panic attack in the consultation room, ultrasonography and electroretinography could not be carried out. Swelling of the upper and lower eyelids made eyelid closure impossible, and exophthalmos, severe corneal ulcer, panophthalmitis, and no light perception were observed (Fig. On presentation to us, the ocular surface of the right eye was covered with pus. Twenty-eight days following second violence, she accepted to undergo ophthalmological examination at our hospital. 
The sharp right eye pain and periorbital swelling gradually deteriorated, and pus began to appear from the right eye. C Hematoxylin and eosin stain of the enucleated eyeball showing large abscess in the anterior chamberįorty-three days after the first visit to our hospital, she was hit again by the husband but continued to endure eye pain at home by using over-the-counter drugs, specifically analgesics, eye drops, and eye ointments. B Clinical photograph showing exophthalmos, severe corneal ulcer, and panophthalmitis. We present this case to raise awareness that eventual panophthalmitis can occur after blowout fracture in the presence of preexisting paranasal sinus infection and delayed specialist consultation.Ī Computed tomography scan of the head showing an old right-sided blowout fracture and sinusitis extending into the inferior of the orbit and into the maxillary and ethmoidal sinuses. Parvimonas micra (previously known as Micromonas micros or Peptostreptococcus micros) is the common causative agent of periodontitis and was cultured from pus samples from the sinus and from the ocular surface. We encountered a case of blowout fracture-related orbital cellulitis with severe corneal ulcer and panophthalmitis that eventually needed enucleation. Meanwhile, since the advent of effective antibiotics, the incidence of severe complications of orbital cellulitis including vision loss, cavernous sinus thrombosis, meningitis, frontal lobe abscess, osteomyelitis, and encephalitis has decreased. It has been presumed that fracture of the orbital floor may impede blood supply to the inferior orbital fat, leading to anaerobic cellulitis. Generally, blowout fracture-related orbital cellulitis can occur following paranasal sinus infection preexisting or occurring within several weeks after the fracture. Recently, spontaneous radiologic improvement in addition to spontaneous clinical improvement was documented in patients with blowout fracture who had been treated conservatively. The indications for and timing of surgical repair of blowout fracture have long been controversial among ophthalmologists, otolaryngologists, and plastic surgeons. The Creative Commons Public Domain Dedication waiver ( ) applies to the data made available in this article, unless otherwise stated in a credit line to the data. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. 
The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. Open AccessThis article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
